Our public health programs are failing the children who need them most.
Together, Medicaid and the Children’s Health Insurance Program (CHIP) cover half of all children who have complex medical and behavioral needs or are at risk of developing them, but the current fee-for-service model doesn’t treat them holistically.
The family doctor doesn’t talk to the physical therapist. The physical therapist doesn’t talk to the behavioral specialist. None of them talk to the school counselor. The burden of coordinating care falls on parents, who spend endless hours meeting with providers, filling out forms, and listening to hold music. For many, it feels like a full-time job.
This flawed system makes it inevitable that some children fall through the cracks.
When providers communicate, young patients get the care they need to stop chronic conditions from worsening. Research shows, for example, that children with autism who begin receiving “psychosocial interventions, speech therapy, and behavioral or pharmacological treatment” before their second birthday have better social and communication skills as adults.
When communication between providers breaks down, kids miss out on those benefits. Children who might have led fairly normal lives with the right preventative interventions end up needing more drastic care. High- and rising-risk youth covered by Medicaid are 56% more likely to visit an emergency room and 53% more likely to be admitted to a hospital, compared to their peers on private insurance. In some cases, children may have to drop out of school or even leave their homes to receive care in institutional settings.
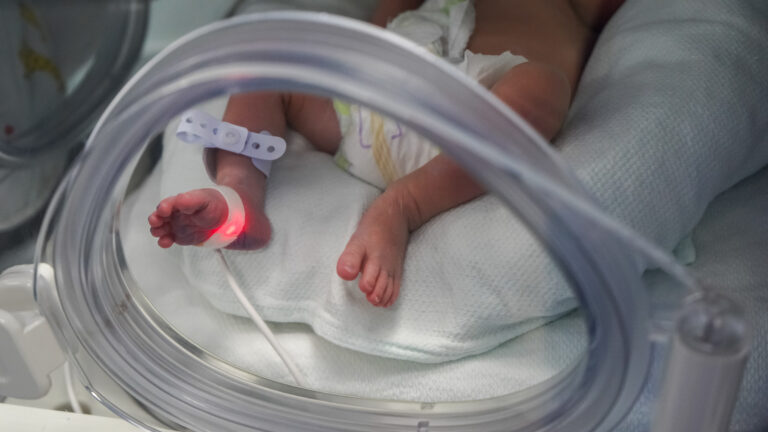
No parent wants to watch their child suffer. That’s why today, the Centers for Medicare and Medicaid Services is announcing a new pilot program to turn this shoddy patchwork of care into a seamless tapestry.
It’s called ASPIRE — which stands for Accelerating State Pediatric Innovation Readiness and Effectiveness — and it will transform how states use Medicaid and CHIP funds to treat “high-risk” youth with complex conditions, as well as “rising-risk” children with risk factors for developing those conditions.
We’ve set aside $125 million to help up to five states test a whole-child approach that connects physical health, behavioral health, and community support over eight years. Coordinating care this way makes it easier to identify warnings signs and provide early interventions that preserve kids’ quality of life.
We’re also shifting away from a fee-for-service model that incentivizes siloed and often expensive treatments rather than the most effective ones. Instead, we’ll provide incentive payments for care teams that harmonize effectively, prioritize prevention, and demonstrate genuine improvements in efficiency, quality of care, and health and functional outcomes.
This kind of care can reshape a child’s future and bring hope to parents who’ve fallen into despair.
The results of our Integrated Care for Kids (InCK) Model, the precursor to ASPIRE, speak for themselves.
“My son has become more sociable, creative, and engaged in sports. He is more aware of his health and, most importantly, happier,” said one parent who participated in InCK.
ASPIRE aims to build on InCK and create more of these success stories by standardizing a more robust value-based payment framework that will give pediatric providers an on-ramp to greater accountability and more substantial rewards for high-quality care.
Parents drowning in a sea of paperwork can also grab a lifeline. ASPIRE will give each family a single point of contact whose North Star is to improve the child’s and family’s overall well-being. States receiving ASPIRE funds must offer parents access to an advice line staffed 24/7 by a medical professional who can access all the relevant information and provide the guidance they need to manage their child’s conditions at home.
The results, we believe, will be transformative: less time spent filling out redundant forms and repeating the same information to six different care providers, faster progress toward health and functional outcomes, and more time for families to enjoy their higher quality of life.
The problems ASPIRE seeks to address are the same ones plaguing American health care more broadly: the focus on reaction rather than prevention, the consistent failure to treat the whole person, the confusing lack of transparency and coordination, and the perverse financial incentives that perpetuate this dysfunction.
Making America Healthy Again is all about innovation. We’re seeking bold new approaches that improve outcomes and reduce costs by tackling chronic conditions with a renewed emphasis on holistic, preventative medicine.
ASPIRE, which will start accepting applications from states later this year, is a small but important part of that larger effort. The initial investment is limited, but for the Americans who benefit from this program, the results could be life-changing. With its unique focus on the pediatric population, ASPIRE has the potential to provide the proof-of-concept we need to help millions of children and families every year. That means lower costs, less strain on families, and more kids who grow up to be healthy, independent adults.
Mehmet Oz, M.D., serves as the administrator of the Centers for Medicare and Medicaid Services. Abe Sutton serves as the director of the Center for Medicare and Medicaid Innovation and deputy administrator for CMS.
