Long before the war, JDC identified a problem few were treating as urgent. Mental health in Israel was not only under-resourced. It was reactive. “We realized we weren’t really addressing prevention,” said Michal Shmul, acting CEO of Resilience and Mental Health at JDC In Israel. “We were focused on treatment, but not on the broader population, not on everyday emotional needs.”
Then came the COVID-19 pandemic. Demand surged. More people, not just those with diagnosed conditions, began searching for support. The insight was clear. Mental health was no longer a marginal issue. It was a universal one. Not a “nice to have,” but a true must-have building block of public health. By the time war broke out, on October 7, that realization had already begun to reshape the organization’s strategy. “We understood we were not talking about a small group,” Shmul said. “We were talking about everyone.”
5 View gallery


Michal Shmul, acting CEO of Resilience and Mental Health
(Photo: JDC in Israel)
The war turned that insight into a national emergency. Israel entered the conflict with a mental health system already stretched thin. Within days, it became clear that traditional care models could not meet the scale of need. Recent data reflects the scale: a majority of children show signs of distress, while large portions of the population report sleep disruption and high anxiety.
“There were not enough professionals, and there would not be enough,” said Yotam Dagan, a clinical psychologist and founder of the mental health app Dugri. “We needed a broad, systemic response, and fast.” For JDC, that meant activating a model it had already begun building: a combination of prevention, technology and cross-sector partnerships. Alongside expanding access to care through professionals and community-based support, the goal was not only to treat trauma, but to prevent it from developing at scale.
Technology became central to that response. JDC established a dedicated mental health division and began identifying, testing and scaling digital and human based solutions that could reach large populations quickly, while maintaining professional standards. “We looked for tools that were already tested, with evidence and real outcomes,” Shmul said. “But we also defined clear criteria. In mental health, if something is not helpful, it can be harmful.”
Another platform for example is “TOKO,” that pairs individuals for ongoing, AI-guided sessions, where structured conversations between peers are designed to build resilience without relying on traditional therapy.
5 View gallery


Nafshi
(Photo: JDC in Israel)
One of the flagship outcomes of that approach is “Nafshi,” a national platform developed as a joint initiative with multiple partners. Nafshi is a digital platform that brings together a wide range of free services tailored to all populations and age groups in Israel. The platform aggregates hundreds of free mental health and wellbeing services and solutions into a single, accessible system, tailored to different populations, languages and needs. A personalized AI agent is also expected to launch soon, designed to help each user find the most relevant support for their specific situation. Since its launch in late 2023, it has recorded more than 200,000 visits, and more than 100,000 have visited since the start of the new war with Iran.
But infrastructure alone is just one part of the story, and it is designed to work alongside human support, not replace it.
JDC’s model is built on a second layer: human connection. That is where Dugri comes in. Originally developed by Dagan, Dugri is a digital platform that creates structured, anonymous peer-support communities. It is not therapy. It is a guided conversation between people who share similar experiences. “The idea is simple,” Dagan said. “People who have gone through similar things understand each other without needing to explain everything.”
For Galit, a clinical dietitian and mother of two, that connection became essential. Her husband has been serving in reserve duty for more than 200 days. “Sometimes he disappears for weeks,” she said. “When he comes back, it’s a bonus, but you can’t build your life around it.” With children studying far from home, declining income and mounting pressure at home, she found herself increasingly isolated. “I told my friends I was struggling,” she said. “I heard, ‘Why are you worried? He’s fine.’ It made me feel like I was complaining too much.”
5 View gallery


Galit, ‘There, I felt understood. No judgment.’
(Photo: Facebook)
She found Dugri through a group for reservists’ spouses. “At first, I just needed a place where I could talk without feeling guilty,” she said. “There, I felt understood. No judgment.” Within days, she was not only sharing but responding to others. Women posted in the middle of the night. Others answered within minutes. Not with clinical advice, but with recognition. “I’m going through the same thing.”
“What we saw was that people don’t just need treatment,” Shmul said. “They need connection. They need to feel they are not alone.”
The impact is not only emotional. It is preventative. Research shows that only a portion of people exposed to traumatic events develop long-term disorders. Early support, normalization, and connections to community can reduce that risk. Dugri’s data reflects that potential. Users report lower stress levels, increased sense of support and improved functioning.
5 View gallery


Yotam Dagan, founder of the mental health app Dugri
(Photo: Social Media)
5 View gallery
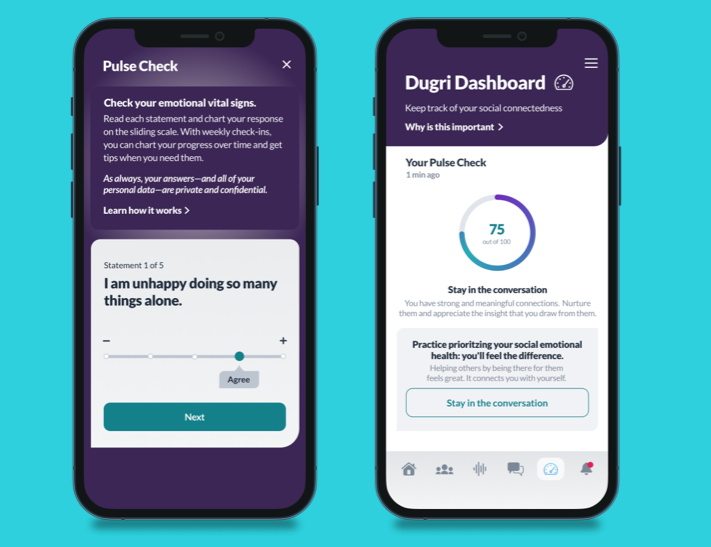

Dugri
(Photo: Dugri Website)
In some cases, the platform has served as a first line of intervention in acute distress. “We had cases where the community responded to someone expressing severe distress,” Dagan said. “People stepped in immediately. That’s the power of peer support.” More broadly, Dugri has become something else: a signal. By analyzing conversations across communities, patterns begin to emerge, frustration, anger, fatigue, difficulty returning to routine. “It’s like a barometer,” Dagan said. “You can see what is happening beneath the surface.”
For JDC, that insight is part of a larger strategy. Technology is not only a delivery tool. It is also a way to understand needs, identify gaps and adapt responses in real time.
The challenge ahead is not short-term. “The war may end, but the psychological impact is just beginning,” Dagan said. “There are hundreds of thousands of people who cannot simply return to normal life.” That is why JDC’s approach extends beyond emergency response.
It combines multiple layers, prevention, community, infrastructure and data, into what Shmul describes as a long-term effort to build national resilience. It also requires coordination across sectors: public, private and social. “In many places, partnership is a slogan,” she said. “Here, it’s the only way this works.”
JDC’s emergency response efforts in Israel are made possible by generous support provided by the Jewish Federations of North America and local Jewish Federations, individuals, families, foundations, and corporations.
As Israel moves into the next phase of the war and beyond it, the frontlines are shifting. From borders to homes. From physical to emotional and the response is being built accordingly. Not only in clinics, but in code. Not only by professionals, but by communities. Because in this war, the question is no longer whether people will need support. It is whether the system can reach them in time.
