“I immediately experience bouts of crying and shaking, a feeling like I’m about to have a heart attack, and the crying just doesn’t stop,” said Ayala Ben Harosh, 57, from Nahariya, describing the anxiety attacks she has faced over the past two and a half years. “It has changed my life, made it unbearable. Everything feels heavy. When my husband isn’t home, I live in the safe room. I also won’t shower if no one else is home, and even then it’s just a five-minute shower.”Shortly after October 7, Ben Harosh was caught in a siren while driving home on the highway. “I pulled over as instructed, and then there were interceptions overhead. I lost control, fainted and found myself in the hospital.” After a second similar incident, she was diagnosed with post-traumatic stress disorder. Since then, she has suffered recurring anxiety attacks. “Every door slam startles me, I begin to shake. This week my husband yawned, and at first it sounded like a siren and I panicked.”
2 View gallery


A shelter in Tel Aviv during a siren
(Photo: AP Photo / Oded Balilty)
Her story reflects the complex reality facing Israeli civilians for more than two and a half years, one that has affected the public’s mental health. Over the weekend, Israel marked one month since the start of the second Iran war, during which more than 82,000 sirens have sounded nationwide — adding to prolonged fighting on multiple fronts.
According to updated Health Ministry data, more than 38,000 people have sought mental health support since the start of Operation Roaring Lion: 28,496 calls to ERAN, a nonprofit emotional support hotline; 6,948 calls to health fund hotlines; and 3,116 inquiries to resilience centers, which provide community-based trauma support. General hospitals have so far reported 333 anxiety casualties. However, officials stress the figures represent only part of the picture, as other organizations also receive inquiries and no comprehensive data exists on how many people experience anxiety symptoms following sirens or rocket impacts. Dr. Gilad Bodenheimer Photo: Ryan Preuss
Dr. Gilad Bodenheimer Photo: Ryan Preuss
Dr. Gilad Bodenheimer, head of the Health Ministry’s Mental Health Division, said the term “anxiety casualties” refers to a broad range of psychological responses to traumatic events, not only classic panic attacks. In the past, most such patients arrived at hospitals, but in recent years — including during the current operation — fewer have sought care in emergency rooms compared to previous conflicts. “This is a positive development,” he said.
He noted that the goal is for people to receive support through hotlines, resilience centers, field responses and community services, easing the burden on emergency rooms. In mass-casualty events, however, hospitals activate special protocols, including opening stress treatment sites, such as the one established at Soroka Medical Center after a missile strike near Arad and Dimona. At the same time, nationwide resilience teams are being reinforced, and initial care is also provided in hotels housing evacuees.
 Dr. Oren Tene Photo: Tal Givoni
Dr. Oren Tene Photo: Tal Givoni
Dr. Oren Tene, director of the psychiatric division at Ichilov Hospital and head of the Mentalix mental health institute, said those who do arrive at emergency rooms are typically people who were physically injured and highly anxious, or individuals coming directly from the scene with acute distress. Treatment varies, he said, as “anxiety casualties” are not a uniform group. “Some experience temporary anxiety due to an acute traumatic event, while others develop severe panic attacks because of prolonged security conditions. It’s important to understand that panic attacks can occur across a range of mental health conditions, including OCD, post-trauma (PTSD) and depression, not just panic disorder.”
Tene explained that treatment in cases of acute anxiety focuses on restoring a sense of safety and control, with medication used only in a minority of cases — when anxiety persists or interferes with sleep and functioning. “The key principle is not to argue with the patient’s experience. Saying there’s no reason to worry or that they should calm down doesn’t help. Anxiety is a very personal experience, and such responses can make patients feel misunderstood.”
“The main goal is to help the person understand that what they are experiencing is very unpleasant, but it will pass and is not dangerous,” he added. “People don’t die from anxiety, don’t faint from it and don’t go crazy — even though these are common fears. Cases of cardiac arrest due to anxiety, despite media attention, are extremely rare.”
A panic attack is defined as an intense, often sudden wave of distress, accompanied by a feeling that something bad is happening or about to happen. “Some people think, ‘I’m about to die,’ ‘I’m about to faint,’ or ‘I’m losing control,’” Tene said. These thoughts are accompanied by physical symptoms, sometimes preceding the attack itself. “The wave combines catastrophic thoughts with physical symptoms such as chest pressure, rapid heartbeat, difficulty breathing or swallowing, shaking and nausea.”
He added that symptoms such as tingling in the fingers and around the mouth, or a cold sensation in the extremities, stem from hyperventilation — when the body enters a heightened “fight or flight” state without acting on it. Other symptoms can include depersonalization and derealization, where a person feels detached, as if observing themselves from the outside or living in a movie.
Bodenheimer noted that in rare cases, anxiety attacks can involve loss of muscle control or even control over bodily functions. Despite the intensity, a single anxiety attack — especially in response to trauma — is not considered an anxiety disorder, which involves recurring episodes. A stress reaction to a life-threatening event falls within the range of normal, he said, though prolonged exposure to repeated trauma increases the risk of conditions such as PTSD, depression and anxiety.
Cecile Prinz, 39, from Kiryat Bialik, has worked in mental health for more than a decade as a social worker and therapist with the Enosh association, which supports people with mental health challenges. She also lives with complex PTSD.
“Feeling unsafe is something I know, but when there’s a real threat, it intensifies,” she said. “Every time there’s an alert and a siren, I feel extreme tension — a racing heart, sweating, shaking, thoughts that I’m losing control, and fear.”
She said the attacks also lead to avoidance. “My mother lives in Haifa — it’s not far — but I haven’t visited her in a month because I’m afraid a siren will catch me on the way. My husband’s workplace agreed to let me come in, and I work from a protected space there. That’s the only way I can maintain a routine.”
 Cecile Prinz Photo: Private
Cecile Prinz Photo: Private
“Living through a period like this, with anxiety attacks at such intensity, is exhausting. It wears down both body and mind,” she said, emphasizing the importance of community support. “When someone sees you, gives you space, reaches out — even just a hug — it matters.”
Tene stressed that panic attacks are self-limiting. “People try to fight the anxiety in every way, but then the body doesn’t learn that it’s a wave that rises and falls on its own. In most cases, an anxiety attack lasts about 30 to 40 minutes.”
Experts say one of the most important factors in coping is the presence of another person. “During anxiety, there’s a sense of losing control, so we look for an anchor — someone stable to help us through, like something to hold onto,” Bodenheimer explained.
Even a stranger’s presence can help, experts say. “Pay attention to people who need help outside,” former hostage Romi Gonen wrote on Instagram last week, describing a severe anxiety attack she experienced on the road during sirens. “I had the most extreme anxiety attack since I returned, and I was alone. Thank God there were good people who immediately stepped in to help me — thanks to them I got through it.”
2 View gallery
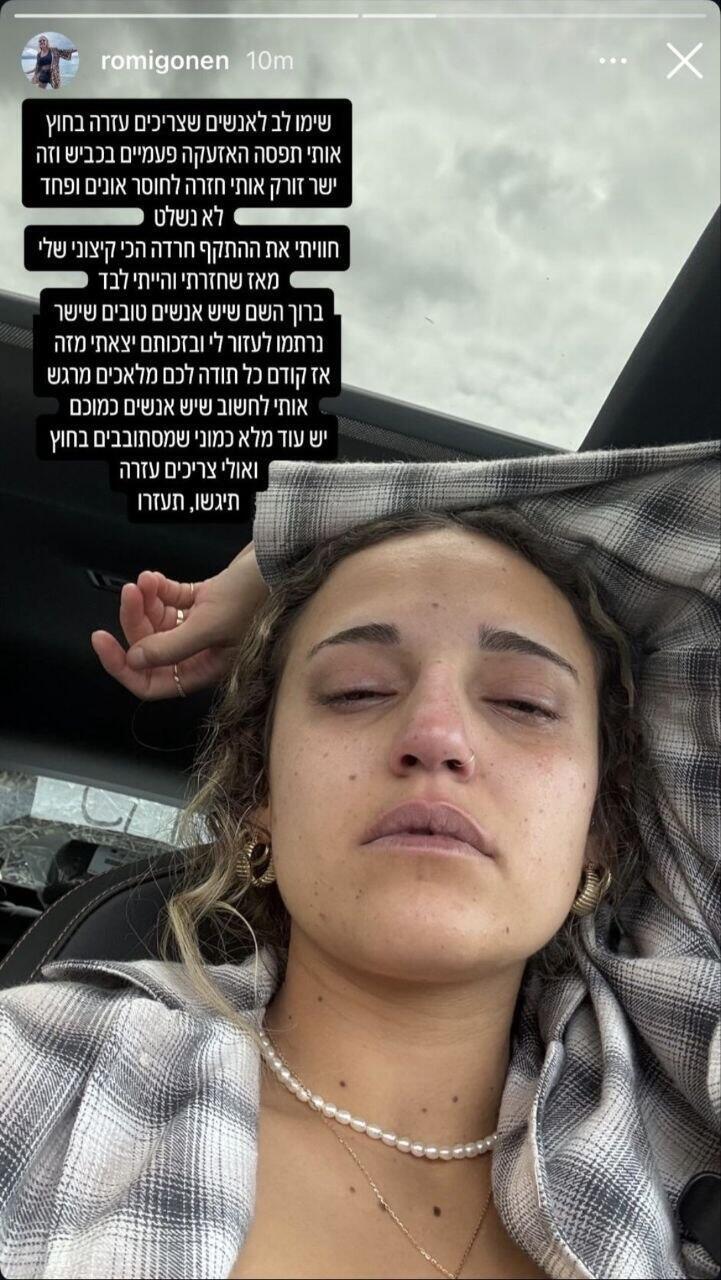

Romi Gonen reveals the difficulty during sirens
(Photo: Instagram)
Tene said human connection is critical. “If someone near you speaks calmly and says, ‘I’m here with you until it passes,’ that alone can be very helpful.” Providing simple explanations about what the person is experiencing can also ease distress, as can helping restore a sense of control.
The Health Ministry recommends immediate assistance during acute trauma using the Ma’aseh model — a Hebrew acronym for a national psychological first aid approach developed by Prof. Moshe Farchi. The model includes four principles: commitment and providing a sense of safety; encouraging effective action; asking simple, grounding questions; and structuring the sequence of events. “In a traumatic event, the first goal is for the person to feel safe and know we are with them,” Bodenheimer said.
“We ask simple questions that activate thinking — such as who was with you, how many people were around — and encourage practical action. This strengthens a sense of control and capability, disconnects from paralyzing emotion and helps the person reconnect to what the brain can process and organize,” he added.
In stressful situations, when there is no immediate danger, Bodenheimer recommends breathing exercises, guided imagery, muscle relaxation, talking with someone close, listening to calming music and even watching familiar content. “I’ve heard of many people returning to beloved comedies these days — from ‘Friends’ to ‘Modern Family’ — shows they know by heart. The familiarity helps and provides relief,” he said.
The health system is preparing for a wave of mental health cases following the fighting. “We have a comprehensive, structured plan, and it will need to continue expanding,” Bodenheimer said in a briefing two weeks ago. Tene noted that psychological responses to dramatic events do not always become clear at the time they occur. Many conditions, such as depression or OCD, do not “take into account” external circumstances and can worsen during or after war. He said there has been an increase in patients experiencing deterioration, including individuals who were previously stable.
If someone around you is in crisis or may be suicidal, do not hesitate — talk to them, encourage them to seek professional help and stress the importance of doing so. You can help them contact community professionals or national support services such as ERAN (dial 1201 or WhatsApp 052-8451201), the SAHAR website or Headspace.
