UnitedHealth Group (NYSE:UNH) has settled a class-action lawsuit over denials of coverage for mental health and substance use disorder treatment. The settlement ends long running litigation related to behavioral health benefits and alleged violations of mental health parity requirements. This resolution comes as the company faces broader regulatory attention on how insurers handle behavioral health care.
For investors looking at NYSE:UNH, this settlement relates directly to a core part of the business: health benefits and managed care, where mental health coverage has been under increasing regulatory and public scrutiny. The case connects to a wider push for mental health parity, in which insurers are expected to treat behavioral health on similar terms to medical and surgical care.
From here, attention will likely turn to how UnitedHealth adjusts its behavioral health policies, internal controls, and provider arrangements. For you, key points to monitor include any impact on litigation risk, regulatory relationships, and the company’s broader efforts to use value based care contracts in mental and substance use treatment.
Stay updated on the most important news stories for UnitedHealth Group by adding it to your watchlist or portfolio. Alternatively, explore our Community to discover new perspectives on UnitedHealth Group.
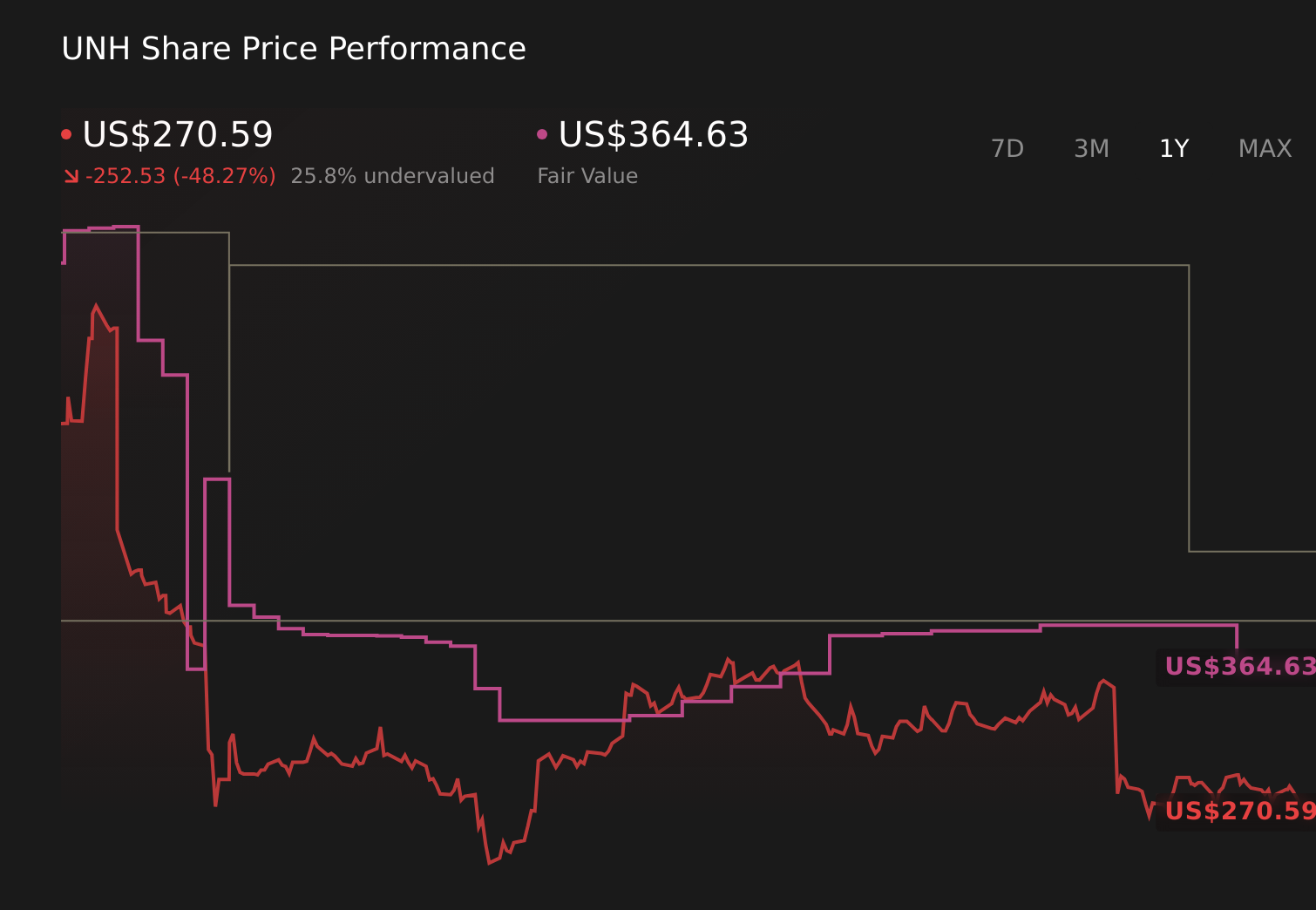 NYSE:UNH 1-Year Stock Price Chart
NYSE:UNH 1-Year Stock Price Chart
The US$1.4 million settlement closes a specific class-action case, but for you as an investor the bigger takeaway is how UnitedHealth Group handles behavioral health compliance and future oversight. The case centered on denials of coverage for residential mental health and substance use treatment, an area where regulators expect tighter alignment with mental health parity rules. With the litigation now dismissed with prejudice, one source of legal uncertainty tied to past practices is removed, while attention shifts to any policy, claims-review, or contracting changes UnitedHealth puts in place to reduce repeat issues.
How This Fits Into The UnitedHealth Group Narrative The settlement links directly to the company’s push into value-based care and predictive programs, because clearer rules around eligible behavioral health services can support more consistent program design over time. It also underlines the regulatory and legal risks already flagged for UnitedHealth, especially as authorities review Medicare Advantage practices at large insurers such as Humana and CVS Health’s Aetna unit. The narrative around technology investment and digital engagement does not fully address how behavioral health coverage rules and parity enforcement could influence member mix, utilization, and margins in coming years.
Knowing what a company is worth starts with understanding its story.
Check out one of the top narratives in the Simply Wall St Community for UnitedHealth Group to help decide what it’s worth to you.
The Risks and Rewards Investors Should Consider ⚠️ Continued scrutiny of mental health parity, together with other ongoing probes, could lead to higher compliance costs or changes in how behavioral benefits are designed. ⚠️ Analysts have already highlighted at least one key risk around the company’s financial position, including debt levels, which could matter if additional fines or remediation spending emerge. 🎁 Settlement with prejudice closes this particular case, which removes the risk of a prolonged legal process and associated uncertainty over this set of behavioral health claims. 🎁 Clearer internal policies on behavioral health coverage could support more predictable utilization patterns, which may help UnitedHealth compare more consistently with peers such as Elevance Health and Cigna. What To Watch Going Forward
From here, keep an eye on any disclosed changes to behavioral health coverage criteria, authorization processes, or value-based contracts, along with follow up commentary from regulators on mental health parity enforcement. Track whether similar lawsuits surface for UnitedHealth or peers, and watch for signals in future filings about legal reserves or compliance investments tied to behavioral health. Those details will help you judge whether this settlement is an isolated clean up of legacy practices or part of a broader reset in how NYSE:UNH manages behavioral health risk.
To ensure you’re always in the loop on how the latest news impacts the investment narrative for UnitedHealth Group, head to the
community page for UnitedHealth Group to never miss an update on the top community narratives.
This article by Simply Wall St is general in nature. We provide commentary based on historical data
and analyst forecasts only using an unbiased methodology and our articles are not intended to be financial advice. It does not constitute a recommendation to buy or sell any stock, and does not take account of your objectives, or your
financial situation. We aim to bring you long-term focused analysis driven by fundamental data.
Note that our analysis may not factor in the latest price-sensitive company announcements or qualitative material.
Simply Wall St has no position in any stocks mentioned.
New: AI Stock Screener & Alerts
Our new AI Stock Screener scans the market every day to uncover opportunities.
• Dividend Powerhouses (3%+ Yield)
• Undervalued Small Caps with Insider Buying
• High growth Tech and AI Companies
Or build your own from over 50 metrics.
Have feedback on this article? Concerned about the content? Get in touch with us directly. Alternatively, email editorial-team@simplywallst.com
