In a landmark case earlier this year, K.G.M. v. Meta Platforms, Inc. et al., a jury held major social media platforms responsible for the mental health harm of an adolescent due to their platforms’ addictive design features. This case underscores growing concerns about adolescent mental health and substance use and draws attention to the factors that may be linked to these concerns. In recent years, a large share of adolescents reported heavy screen time and social media use, trauma exposure – including direct and indirect exposure to gun violence – loneliness, and sleep deprivation. These experiences are tied to poor mental health outcomes, including anxiety and depression. Meanwhile, suicide death rates remain high among adolescents and overdose deaths reached record numbers amid the opioid epidemic.
To address growing mental health and substance use concerns several measures were introduced. This includes the 2022 Bipartisan Safer Communities Act (BSCA), which allocated funds to strengthen school-based mental health services, particularly in high-need areas, and utilize Medicaid to expand youth services. In 2021, the U.S. Surgeon General declared a youth mental health crisis and released an advisory outlining a wide range of recommendations to support this population. However, recent policy actions under the second Trump Administration have rolled back some of these efforts. Funding for school-based mental health services via the BSCA was disrupted, prompting questions about how to retain school mental health providers and reach students in need. Other, large-scale changes to insurance are expected to negatively impact coverage and access to care in the coming years. This includes changes to Medicaid, which provides coverage to nearly 40% of children and teens. Additionally, the President’s budget for 2027 proposes cuts to agencies engaged in mental health and substance use disorder services, including ongoing efforts to restructure SAMHSA. SAMHSA also oversees the 988 crisis hotline – which was recently linked to decreased adolescent suicide mortality. Funding for 988 remains flat in 2027, though previous actions have already impacted services, including the removal of an extension line to assist LGBTQ individuals. LGBTQ youth are more likely to experience suicidality compared to their peers.
This brief analyzes the latest data (2024) from the CDC WONDER mortality database and the National Survey on Drug Use and Health to examine the prevalence of adolescent mental health conditions and substance use, related deaths, and access to behavioral health services.
1. Despite some modest improvements, many adolescents experience poor mental health and substance use issues.
In 2024, 15% of adolescents (or 3.8 million) reported a past year major depressive episode (MDE) and 19% (or 4.9 million) reported moderate to severe symptoms of anxiety (Figure 1). The share of adolescents with an MDE decreased from 21% in 2021 during the pandemic – the oldest trend data available – to 15% in 2024. Additionally, a survey of high school students found that the share of students reporting feelings of sadness and hopelessness – which can be indicative of depressive disorder – increased from 30% in 2013 to 42% in 2021, before slightly declining to 40% in 2023. While NSDUH data on anxiety cannot be trended over time, other survey data suggest that diagnosed anxiety has increased over time among adolescents, with prevalence remaining higher than pre-pandemic levels. Anxiety is the most common mental health condition in this population.
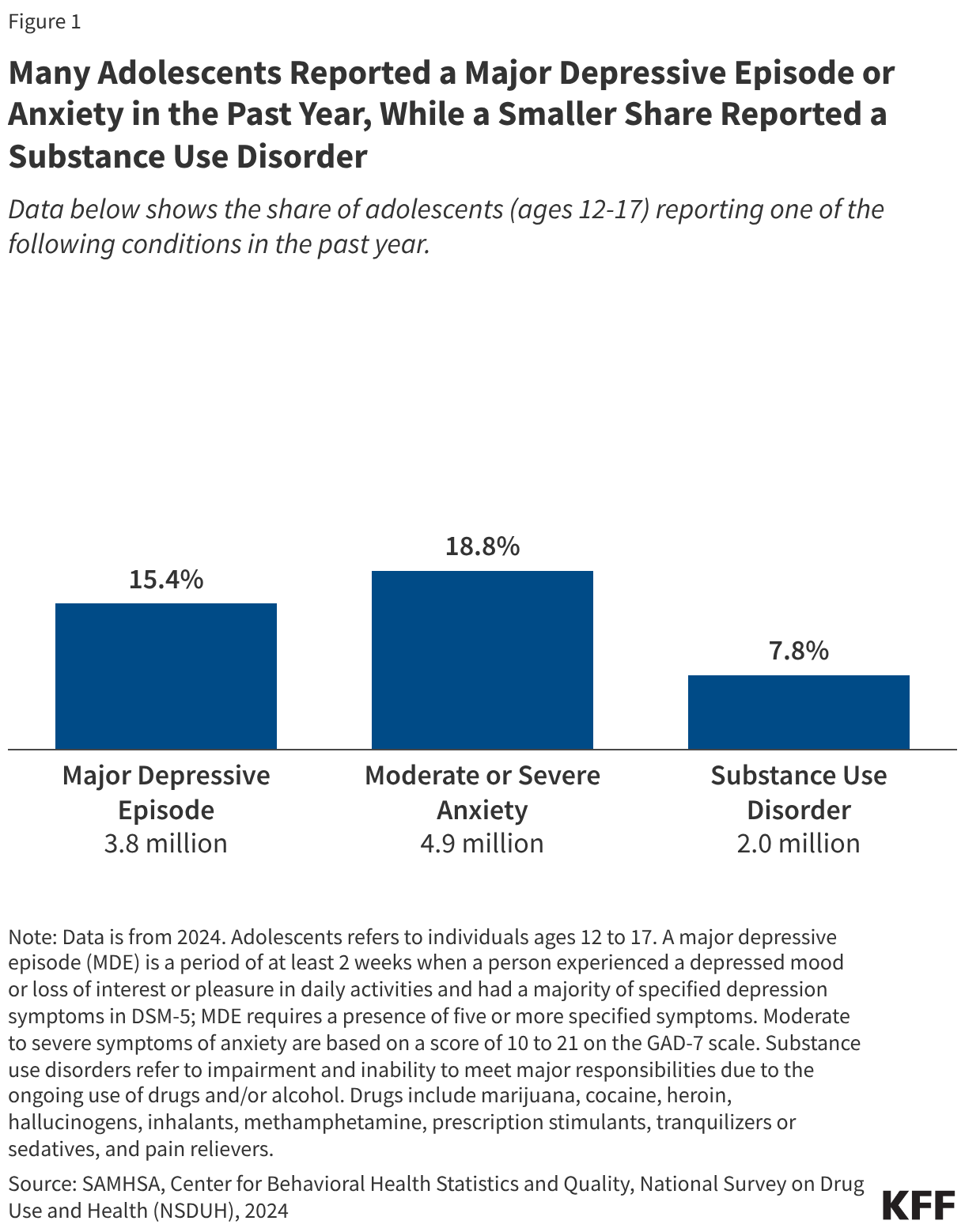
In 2024, 7.8% (or 2 million) adolescents reported having a substance use disorder in the past year (Figure 1). This is a slight decrease from the 9.2% of adolescents reporting a past year substance use disorder in 2021 – the oldest trend data available. A prior KFF analysis found that the use of drugs and alcohol among high school students slightly declined from 2017 to 2023, despite the surge in drug overdose deaths during pandemic years.
Among adolescents with mental illness and/or substance use disorder, over half have private insurance and 4 in 10 have Medicaid. However, Medicaid is a major payer for mental health and substance use services for youth. Medicaid can facilitate access to care in schools and its Early and Periodic Screening, Diagnostic and Treatment (EPSDT) benefit requires coverage of medically necessary services and maintains low out-of-pocket costs.
2. Substance use is higher among adolescents with mental illness compared to adolescents without mental illness.
In 2024, the use of any illicit drug was significantly higher among adolescents with a past year MDE than their counterparts (33% vs. 12%); and among adolescents with symptoms of anxiety than their counterparts (26% vs. 10%) (Figure 2). The co-occurrence of poor mental health and substance use is common. In a CDC convenience sample survey of teens, ages 13 to 18, who used substances in the last 30 days, 40% reported using substances to cope with anxiety or depression.
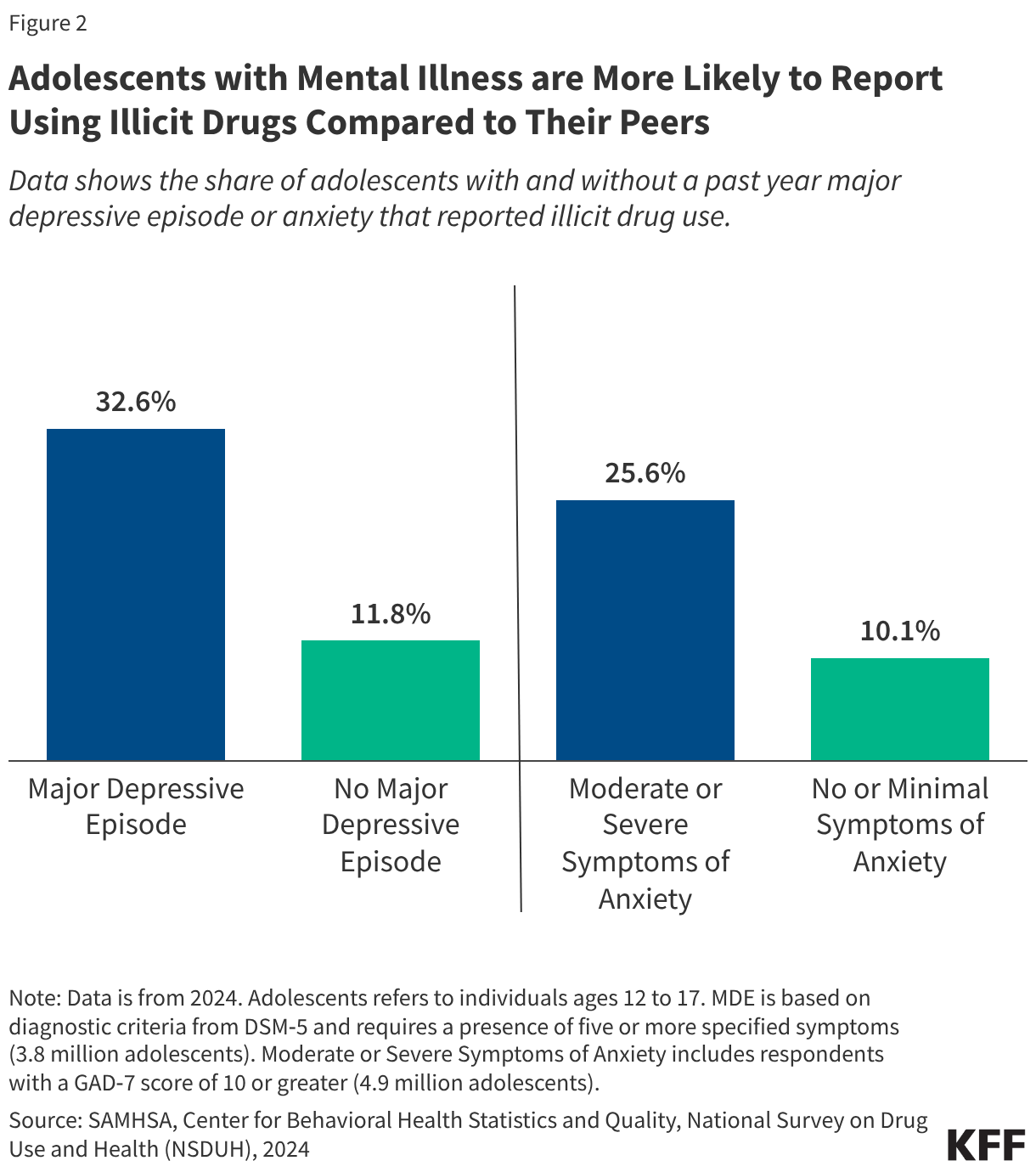
Marijuana, a drug that is now legally available to adults in many states, has been linked to the onset of psychoticdisordersamong youth, and is used by a large share of adolescents with an MDE (25%) and adolescents with symptoms of moderate to severe anxiety (18%). Adolescents without a past year MDE or anxiety were significantly less likely to report marijuana use (8% and 7%, respectively). Marijuana use among adolescents is associated with earlier onset of psychosis, with more frequent use linked to increased risk of adverse mental health outcomes, including schizophrenia. Further, the presence of the compound THC in marijuana has increased over time and is linked to psychotic symptoms and disorders.
3. Suicide deaths among adolescents are slowly trending downward but remain higher than a decade ago.
In the past decade, adolescent suicide deaths increased and peaked in 2018 (1,750 deaths), followed by a gradual decline through 2024 (1,478 deaths, Figure 3). There was a 5% decrease in adolescent suicide deaths from 2023 to 2024 (1,555 vs. 1,478). These deaths are more prevalent among adolescent males and are more rapidly increasing for adolescents of color compared to their White peers. Although suicide deaths are higher for adolescent males than their peers, serious thoughts of suicide are higher for adolescent females. Data on the suicide deaths was not available by LGBQ+ identity. However, LGBQ+ youth are more likely to report suicidality than their heterosexual peers. It is possible that some suicides are misclassified as drug overdose deaths since it can be difficult to determine whether drug overdoses are intentional.
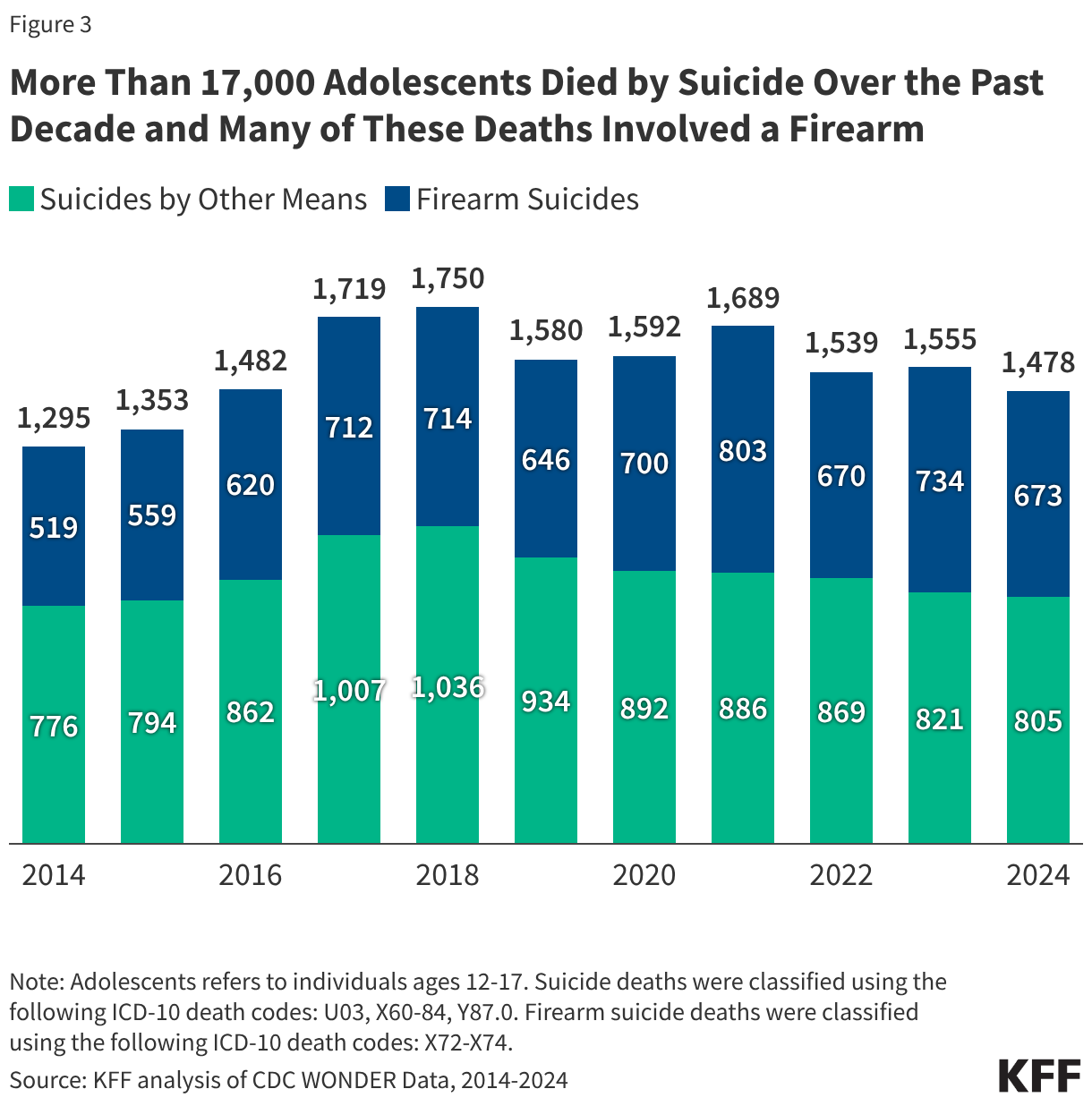
More than 17,000 adolescents died by suicide over the past decade and over 4 in 10 of these deaths involved a firearm (Figure 3). Access to firearms, particularly in the home, is a risk factor for suicide deaths among children and adolescents.
4. After surging during the pandemic, drug overdose deaths among adolescents sharply declined in 2024 but remain above pre-pandemic levels.
The sharp decline in drug overdose deaths among adolescents was driven by a reduction in opioid-related deaths: 557 deaths in 2023 vs. 272 in 2024 (Figure 4). Despite decreases in substance use among adolescents, adolescent drug overdose deaths more than doubled during the COVID-19 pandemic. This shift was largely due to drugs laced with opioids, particularly the synthetic opioid, fentanyl. Opioid-related deaths among adolescents jumped from 165 in 2019 to 396 in 2020 and continued to increase for several years before declining by approximately 50% between 2023 and 2024 (from 557 to 272, Figure 5). These trends mirror broader trends in opioid-related deaths across the total U.S. population.
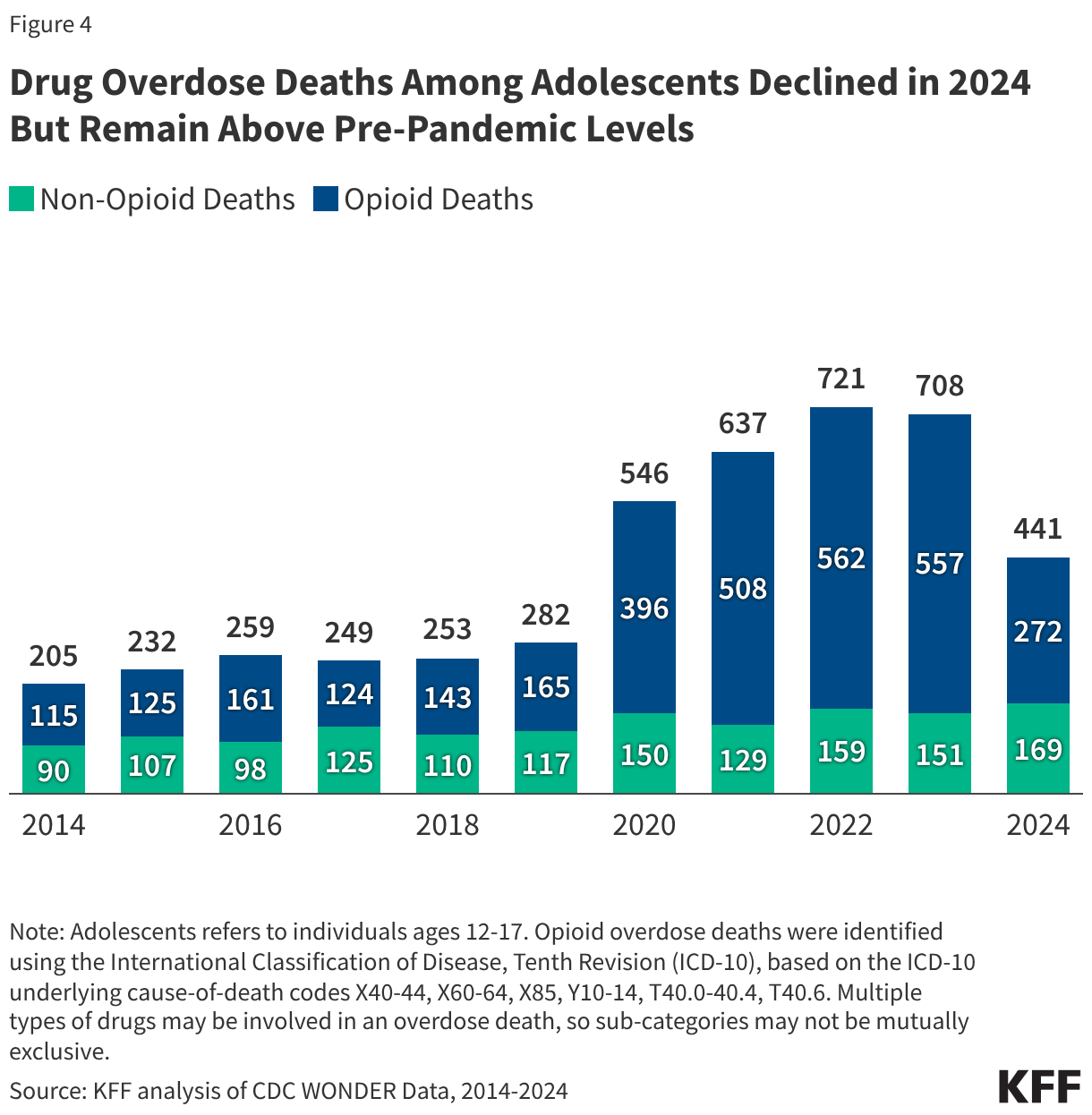
Multiple actions may have contributed to the decline in overdose deaths, including school-based initiatives for youth. Policy actions implemented in response to the opioid epidemic include expanded access to treatment, public awareness campaigns, and improved fentanyl detection. Schools have also responded to the overdose crisis in multiple ways. For example, in the 2024-2025 school year, 52% of public schools offered fentanyl education to students and 77% stored naloxone – a nasal spray to reverse opioid overdose. However, challenges remain, such as adolescents obtaining drugs through social media which may be contaminated with fentanyl.
5. Adolescents receive mental health services in a variety of settings, including schools; however, recent policy changes may affect access in the future.
Six out of ten adolescents with a past year MDE reported receiving mental health treatment in 2024 (Figure 5). Many of these adolescents report receiving outpatient care in a variety of settings, including through telehealth treatment (33%). Thirty-one percent of adolescents with a past year MDE report taking prescription medication (31%).
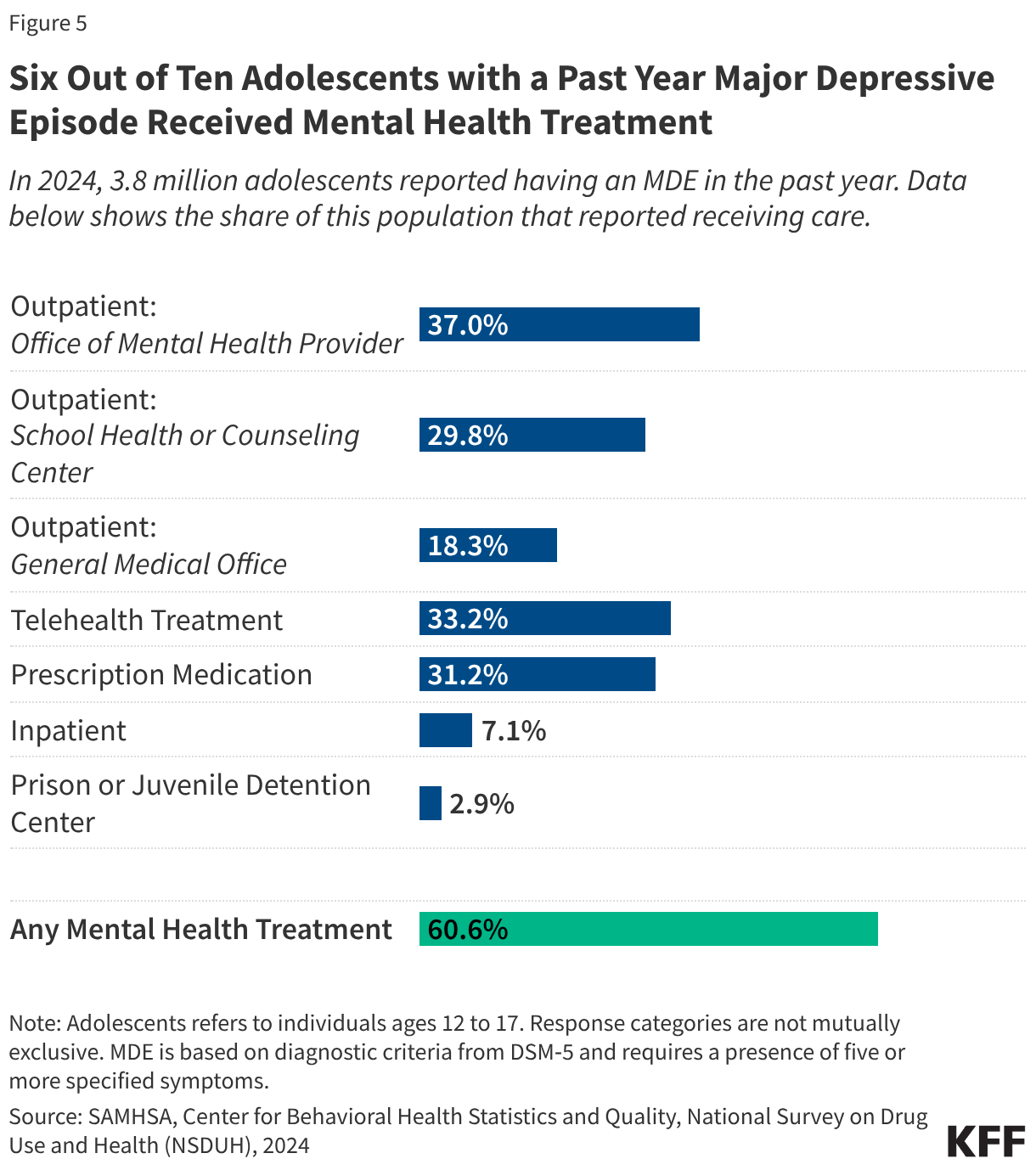
Approximately 3 in 10 youth with a past year MDE obtain care through school health or counseling services; however, changes in funding put access to school-based mental health services at-risk. During the second Trump Administration, ongoing policy changes may impact youth access to mental health services. This includes rolling back funds to broaden access to mental health and trauma services in schools that were originally allocated through the Bipartisan Safer Communities Act.
Among the 2.4 million adolescents in need of substance use care in 2024, only 30% received treatment. This may be linked to limited access to buprenorphine and residential addiction treatment facilities among this population. Additionally, many residential addiction treatment facilities do not have availability for adolescents and are costly. These facilities often do not provide buprenorphine to adolescents with opioid use disorder.
This work was supported in part by the Philos Foundation. KFF maintains full editorial control over all of its policy analysis, polling, and journalism activities.
