After the deadly event, local leaders have pointed to Oregon’s mental health system and civil commitment laws, where very few people qualify for forced treatment.
PORTLAND, Oregon — In the wake of a car bombing at the Multnomah Athletic Club that avoided greater catastrophe by mere “luck,” officials have since pointed to driver Bruce Whitman’s documented mental health challenges and Oregon’s civil commitment laws — asking why Whitman wasn’t forced into mental health treatment.
Whitman did give up guns to law enforcement under extreme risk protective orders, better known as a “red flag” law, but he turned down referrals for mental health treatment and failed to qualify for involuntary care.
While Whitman’s actions and thought process behind the bombing cannot be definitively linked solely to mental illness, KGW can explain why so few people qualify for civil commitment or forced mental health treatment — a topic that we’ve covered extensively for years through our “Uncommitted” series.
The high bar for forced care
On Monday, Multnomah County District Attorney Nathan Vasquez said Whitman’s death and the MAC bombing provided a “sad example” of gaps in the state’s mental healthcare system.
“We need a system that serves those who are suffering from mental illness in a way that is more long term, more in-depth,” Vasquez said. “I really believe we need to do more than what our civil commitment laws currently provide.”
Civil commitment includes a high legal bar, as it takes away a person’s rights to their own healthcare choices. More than 90% of mental health holds in Multnomah County don’t meet legal criteria upon review by doctors, county investigators and judges.
“On the other hand, a feature of a lot of these mental illnesses is you don’t think you have a mental illness,” said Sgt. Josh Silverman of the Portland Police Bureau, who leads the agency’s behavioral health unit. “To rely on voluntary engagement when you don’t think you have a mental illness is problematic as well.”
For years, KGW has shared stories of families who struggled to get their loved ones into treatment.
“We’re the monsters, we collectively we didn’t help this person who needed help,” said Jeff Rott, the father of a man who flew to New York while in psychosis and received care there that he hadn’t received in Oregon.
The challenge is, civil commitment is now extremely rare in Oregon.
Fewer than five people a month are admitted to the Oregon State Hospital on civil commitment orders.
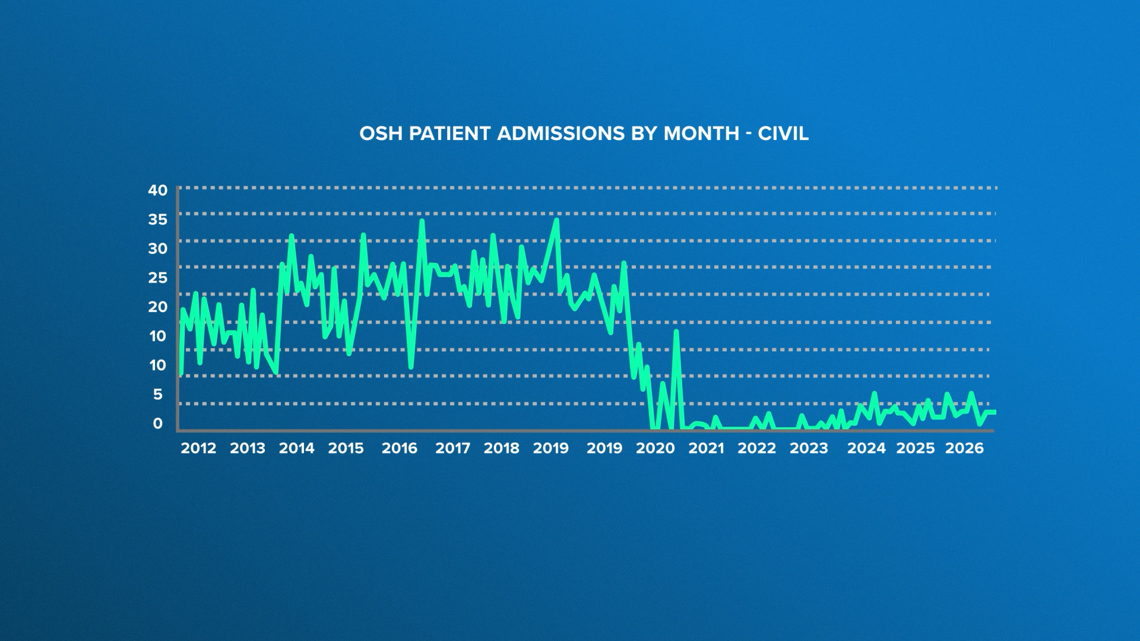
Crowding and criminal commitments
Over the last decade, the state’s priorities have flipped. Most OSH patients are criminal defendants ordered to receive treatment so they can “aid and assist” with their own defense.
The state prioritizes these cases due to federal requirements and a contempt order that is costing Oregon millions of dollars. Though there are efforts underway to increase capacity at OSH, it’s not proceeding quickly enough to make room for both civil and criminal patients.
As a result, civil commitment treatment spots are limited, leading Oregon to effectively wait for someone to be charged with a crime before committing them to secure psychiatric care.
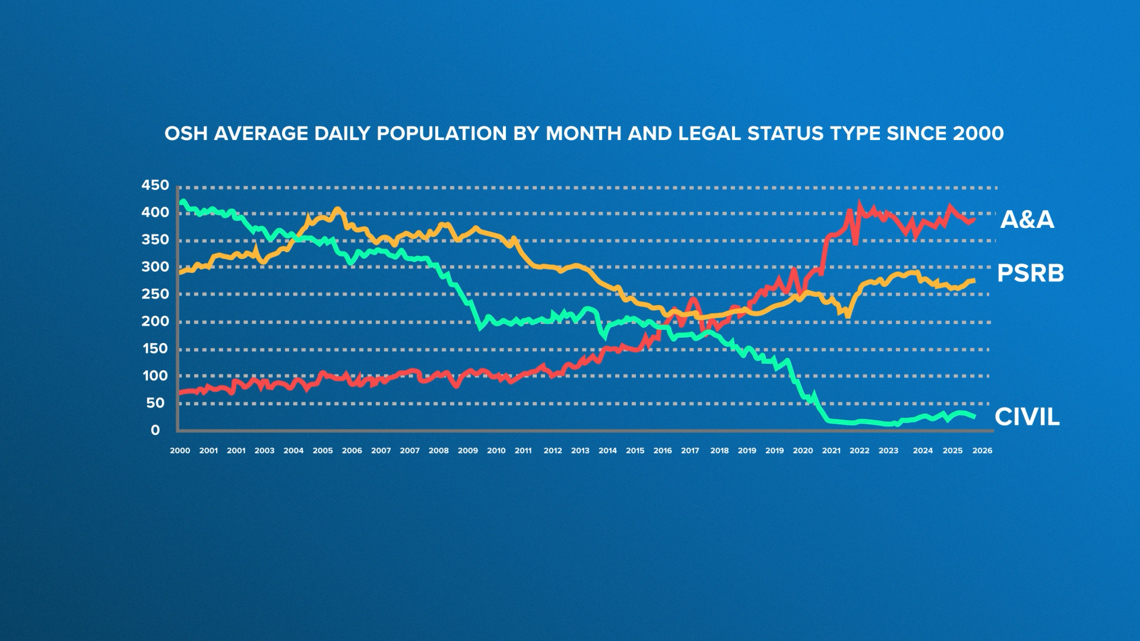
“(Criminal charges are) often the only pathway someone has toward some level of mental health treatment — that is an absurd way of approaching this issue,” said Washington County District Attorney Kevin Barton in a previous interview with KGW.
Many political leaders, judges and mental health advocates have said the best strategy is to build more treatment options in local communities for early intervention.
“Everybody wants a fix that can happen tomorrow that’s very simple, and it feels like involuntary treatment is the answer, but the reality is that we need to build out our voluntary treatment,” said Tom Stenson with advocacy group Disability Rights Oregon.
However, community treatment often relies on people choosing to accept treatment options. Bruce Whitman’s family members and Portland police said he repeatedly turned down treatment referrals.
The Oregon state legislature last year passed House Bill 2005 — a new that went into effect in January, lowering the bar for civil commitment. Instead of requiring “imminent” danger to oneself or others, judges can now consider past or future behavior.
Multiple sources told KGW it’s too early to identify any clear effects from the law change, such as if more people have been deemed eligible for civil commitment as a result of the relaxed standards.
However, there is still a problem of space. If the Oregon State Hospital is at capacity, where would judges send a potentially growing number of people who qualify for forced mental health treatment? That remains to be seen.
A civil commitment typically involves four major steps:
Mental Health Hold: a family or community member could trigger a law enforcement review and temporary hold for a mental health evaluation at a hospitalNotice of Mental Illness: a medical decision, a doctor could find enough cause for a person to move forward in the civil commitment process as they are a danger to themselves or othersInvestigation and hearing decision: a county behavioral health investigator has three days to respond to an NMI, talking to a patient and determining if their symptoms meet standards for a judicial hearing within five business daysJudicial ruling: a judge oversees a hearing where they would rule if the person meets the legal standards for civil commitment — up to six months of involuntary mental healthcare.
